For many years, patients experiencing lingering symptoms long after treatment for Lyme disease often found themselves facing skepticism, both from the medical community and broader public. These individuals reported chronic fatigue, joint pain, cognitive difficulties, and neurological issues, even after completing standard antibiotic therapies. While these symptoms were real to patients, the concept of “chronic Lyme disease” remained contentious in the world of medicine. Today, however, there is a noticeable shift in how the condition is being acknowledged and addressed by healthcare professionals.
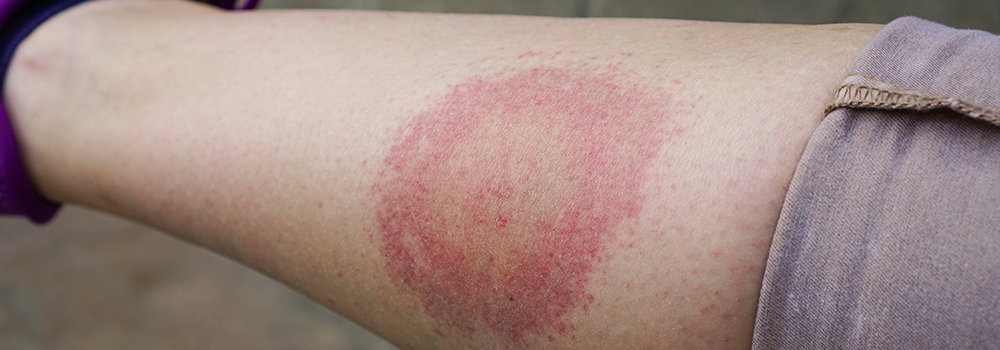
Lyme disease, resulting from the bacterium Borrelia burgdorferi and spread by the bite of infected blacklegged ticks, stands as the most prevalent vector-borne illness in the United States. Initial signs often encompass fever, tiredness, headache, and a distinctive skin rash. If diagnosed promptly, the condition is usually manageable with antibiotics. Nonetheless, a significant number of individuals experience symptoms that linger even after therapy. These ongoing symptoms have sparked years of discussion regarding what is currently referred to as “Post-Treatment Lyme Disease Syndrome” (PTLDS).
The term PTLDS is increasingly favored among clinicians as it distances the diagnosis from controversial connotations associated with “chronic Lyme disease” while acknowledging that a subset of patients do continue to suffer long-term effects. Recent years have seen a growing number of doctors who are open to the idea that these post-treatment complications warrant medical validation and active management, rather than dismissal or psychosomatic attribution.
A contributing factor to the changing viewpoint is the gathering of patient-reported information and medical research indicating that a more intricate process occurs in the body after infection. Scientists are investigating multiple hypotheses, such as immune system imbalance, residual bacterial particles causing inflammation, or even the possible influence of additional infections carried by ticks. Although no single theory has achieved widespread agreement yet, the growing body of evidence has paved the way for more research.
Another reason for this shift in attitude is the increased visibility of Lyme disease itself. With climate change expanding the habitat of ticks, cases have surged in regions previously considered low risk. More people, including physicians and public health officials, now know someone affected by persistent Lyme-related issues, lending the condition a greater degree of legitimacy and urgency.
The conventional method for addressing Lyme disease typically involves administering antibiotics for several weeks. This approach proves successful for numerous individuals, though not for every patient. Those who continue to experience symptoms often feel frustrated when test results indicate no ongoing infection, and physicians find it challenging to provide effective solutions. This situation has contributed to the emergence of a medical gray area, where patients switch between specialists or resort to alternative treatments beyond conventional medicine. Regrettably, the absence of uniform medical direction has occasionally exposed patients to unvalidated therapies or potential medical exploitation.
Recognizing these gaps, certain healthcare organizations are starting to establish specialized centers devoted to tick-borne diseases and ongoing Lyme symptoms. These initiatives seek to provide a more holistic approach to care, integrating neurology, immunology, and rehabilitation into their treatment strategies. Moreover, they prioritize acknowledging patient experiences and affirming their symptoms, even when conventional diagnostic methods are insufficient.
Still, not all corners of the medical world have embraced the shift. There remains skepticism about whether ongoing symptoms are directly caused by Lyme disease or result from other conditions or psychosomatic responses. Critics of the “chronic Lyme” label argue that misdiagnosis could lead patients down a path of unnecessary treatment or missed detection of other health issues. However, proponents of broader recognition argue that dismissing persistent symptoms leaves patients unsupported, often worsening their condition due to stress, delayed care, or emotional strain.
Insurance coverage is one more challenge. Numerous health plans restrict their coverage to brief antibiotic treatments and do not offer reimbursement for prolonged therapies or integrated medical care, citing a lack of sufficient evidence. As awareness of PTLDS increases and new research projects gain financial support, it is possible that future medical guidelines will adapt to more accurately address the requirements of these patients and enhance access to care.
At the heart of the issue is a growing awareness that complex illnesses like post-treatment Lyme disease don’t always fit neatly into traditional diagnostic boxes. Just as the medical field has slowly come to understand the lingering effects of COVID-19, there is increasing recognition that infectious diseases can sometimes lead to long-lasting health challenges that extend well beyond the resolution of the acute infection.
In the meantime, patients experiencing persistent symptoms after Lyme treatment continue to seek answers, often navigating a difficult journey of advocacy, trial and error, and fragmented care. The ongoing evolution of medical understanding offers a glimmer of hope—not only for validation, but for more effective treatments, increased funding for research, and a greater emphasis on whole-patient care.
As awareness of Lyme disease expands and research delves further into its enduring effects, the distinction between skepticism and diagnosis might soon become less distinct. This transition is a crucial move towards establishing a more empathetic, knowledgeable, and scientifically-based method for addressing the needs of those whose struggles have long been overlooked.